Cardiovascular disease (CVD) is a term that refers to various conditions that affect the heart and blood vessels. These conditions can range from ‘simple’ problems like high blood pressure to more serious issues like heart attacks and stroke. CVD is the major cause of morbidity and mortality worldwide, so it is important to understand the various risk factors and mechanisms behind the development of these conditions. With proper care, CVD can be easily mitigated, if not avoided entirely. At NutriFix, we believe that it should not bear the crown as the number 1 killer disease worldwide.
In this article, I’ll go over some of the key points about CVD, including the process of artherosclerotic plaque formation, the role of dysfunctional HDL, and the spill-over effects of increased CVD risk on other diseases. I’ll also talk about some of the genetic predispositions that can influence CVD risk, and how these can be addressed through a combination of behavioral tools, nutrition, and supplements. Ready? Let’s go!
EL.. DL
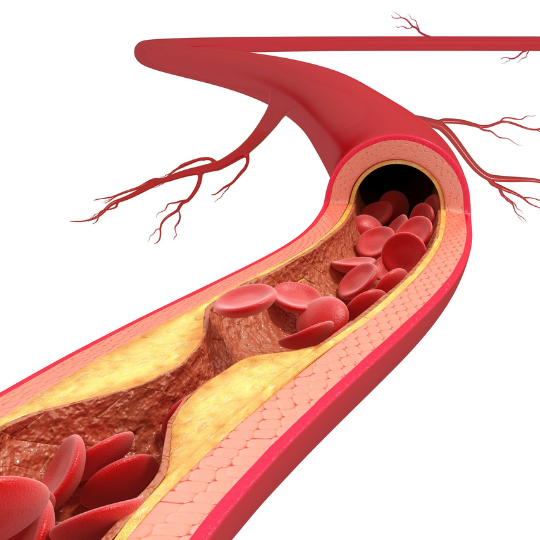
One of the main risk factors for CVD is high LDL cholesterol, which is often referred to as “bad” cholesterol. When LDL cholesterol levels are too high, it can accumulate in the walls of the arteries, forming plaques. These plaques can narrow the arteries and make it more difficult for blood to flow through them, which can lead to a variety of problems including heart attacks and stroke.
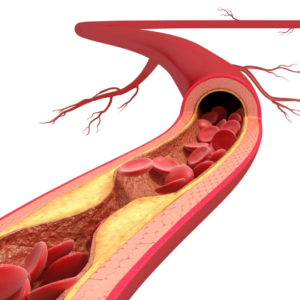
The process of artherosclerotic plaque formation involves several key steps. First, LDL cholesterol is oxidized, which makes it more likely to stick to the walls of the arteries. Next, macrophages, which are immune cells that help to clean up debris in the body, are attracted to the site of the plaque. These macrophages engulf the LDL cholesterol, forming foam cells. Over time, these foam cells can accumulate and form a plaque.
The “good” lipoprotein: HDL
Another important factor in the development of CVD is dysfunctional HDL, which is often referred to as “good” cholesterol. One of the main functions of HDL is to transport excess cholesterol from the arteries back to the liver, where it can be broken down and eliminated from the body. This process is known as reverse cholesterol transport. However, if the HDL is dysfunctional, it may not be able to carry out this important function effectively, leading to a build-up of cholesterol in the arteries.
High blood pressure and smoking are two additional risk factors for increasing CVD risk, due to their detrimental effect on blood vessels, already under the cholesterol stress described above. Generally speaking 2 out of these 3 main CVD risks (altered cholesterol, high blood pressure and smoking) should trigger an alarm signal. But in all fairness, if you aim for optimal health, none of these risk factors should really be left unaddressed in your life!

CVD can also have spill-over effects on other diseases. For example, people with CVD are at increased risk of developing diabetes, as high levels of LDL cholesterol can lead to insulin resistance. CVD can also increase the risk of developing other conditions such as kidney disease and certain types of cancer. So in essence you want to avoid CVD at all costs!
What about your genes?
Briefly, there are several single nucleotide polymorphisms (SNPs) in key genes that have been associated with an increased risk of CVD, like the APOE gene and the PCSK9 gene. In the first instance, these genetic predispositions can be addressed through a combination of behavioral tools, nutrition, and supplements. Depending on the severity of the situation, various classes of drugs can also be considered to lower any CVD risk that cannot be otherwise mitigated.
Behavioral tools that can help to reduce CVD risk include things like getting regular exercise, managing stress, and getting enough sleep. Sounds too general and obvious, but these can all really help to improve cardiovascular health and reduce the risk of developing CVD. How much of each, in what proportions and how to implement any changes? Well, this is what we’re here for: to guide you through your genetic and metabolic optimization journey.
In terms of nutrition, there are certain foods that have been shown to be particularly beneficial for heart health. These include foods that are high in fiber, such as fruits, vegetables, and whole grains, as well as foods that are rich in antioxidants, such as berries and nuts. Omega-3 fatty acids, which are found in fatty fish like salmon, can also help to improve cardiovascular health.

Several supplements have also been shown to be helpful in reducing CVD risk. These include supplements like fish oil, which is high in omega-3 fatty acids, Coenzyme Q10, which is an antioxidant that helps to protect the heart, grape seed extract, pine bark and a few others. Which are the best for you and what is the best supplemental protocol you should consider? Reach out, let’s have a chat and we can decide together!