Lately, “Gut health” has gained a lot of fame and is not for nothing. Gut health refers to gut microbiome balance and correct functions. The Gut microbiome is the community of beneficial bacteria that lives in your intestines; it helps with digestion, absorption and the production of beneficial compounds by fermentation. An imbalance between bad and good bacteria leads to gut microbiome dysbiosis, which alters the composition and function of this community in the digestive tract. This can have significant impacts on your health (Barko PC, et al 2018).
Gut dysbiosis can be identified by different markers which include the identification of compounds produced by each bacterial species or bacterial cultures. If there are high concentrations of Bifidobacterium and Lactobacillus, the microbiome is healthy. If there is a high concentration of pathogenic bacteria, such as Escherichia coli and Staphylococcus aureus, there is dysbiosis. Also, imbalances in the ratio of Firmicutes to Bacteroidetes and Proteobacteria have been associated with dysbiosis (Barko PC, et al 2018).
But what are the potential causes of gut microbiome dysbiosis?
The main factor is diet. A diet high in processed, sugary foods and low in fiber can disrupt the balance of the gut microbiome and lead to dysbiosis. Inflammation can also contribute to dysbiosis. Inflammation can be caused by chronic stress, infection, or the use of medications. Also uncontrolled enemas or other interventions could alter the normal microbiome (Barko PC, et al 2018).
Gut dysbiosis and diseases
Neurodegenerative diseases
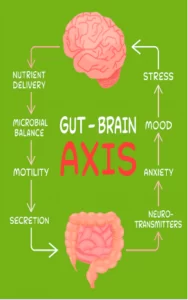
There is a growing body of evidence linking gut microbiome dysbiosis to neurodegenerative diseases. This connection is thought to occur through the microbiota-gut-brain axis, a complex network of communication between the gut microbiome, the enteric nervous system, and the central nervous system. Dysbiosis in the gut microbiome has been linked to a variety of neurodegenerative conditions, including Alzheimer’s disease, Parkinson’s disease, and multiple sclerosis (Caputi V, et al, 2018).
Atherosclerosis
Another factor that has been linked to dysbiosis and an increased risk of atherosclerosis is the conversion of carnitine and choline to trimethylamine (TMA) and trimethylamine N-oxide (TMAO). This process is thought to be influenced by the gut microbiome, and high levels of TMAO have been associated with an increased risk of cardiovascular disease. However, there are potential strategies that may help to mitigate this risk. For example, increasing intake of dietary fiber and fermented foods has been shown to promote a more balanced gut microbiome and reduce TMAO levels (Barrington WT, et al, 2017).
Inflammation
Lipopolysaccharides (LPS) are molecules found on the outer surface of some bacterial cell walls, and they can trigger immune responses when they leak into the bloodstream, causing chronic inflammation and increasing the risk of dysbiosis. But to counteract this, short chain fatty acids (SCFAs) come into the scene. SCFAs are produced by the fermentation of dietary fibers by the gut microbiome, and they have anti-inflammatory properties. Inflammation and dysbiosis can be produced if there are more LPS than SCFA in the bloodstream. In the next paragraphs, we are going to explain how you can increase your SCFA by fermentation (Camille Martin-Gallausiaux, et al, 2021).
Genetic predispositions
There is growing evidence that certain genetic predispositions can influence an individual’s risk of developing gut microbiome dysbiosis. Some examples are:
- FUT2 gene: this gene codes for the enzyme that is involved in the synthesis of H antigens in the gut. Single nucleotide polymorphisms (SNPs) in the FUT2 gene have been linked to variations in the gut microbiome composition and an increased risk of dysbiosis.
- PGLYRP2 gene: this gene codes for peptidoglycan recognition proteins. These proteins are responsible for binding bacterial metabolites in the intestine and keeping intestinal homeostasis. SNPs in this gene have been related to intestinal infections and inflammatory bowel disease, and recently it has been identified that people with this SNP are more likely to develop Parkinson’s disease (Gorecki AM, et al, 2020).
Nutrition and lifestyle
As always, just because you have certain SNP, it doesn’t mean you are going to develop a disease. Nutrition and lifestyle play an important role in your health. Here are some recommendations to keep your gut healthy:
- Sun and light exposure: research has shown that exposure to sunlight and outdoor environments can help to promote healthy gut microbiome, while sedentary behavior and artificial light at night may be detrimental (Barko PC, et al 2018).
- Regular physical activity and mindfulness: techniques such as meditation and deep breathing may also be beneficial (Barko PC, et al 2018).
- Nutrition: there are certain foods that could support a healthy gut microbiome:
- fermented food rich in beneficial bacteria, such as sauerkraut, kimchi and kombucha*
- high-fiber plant-based foods that help with the production of SCFA by fermentation such as vegetables, fruits, nuts, and seeds
- prebiotic foods which provide fuel for the growth of beneficial bacteria like onions, garlic, and leeks (Barko PC, et al 2018).
- Supplementation: specific probiotics and prebiotics may also be useful for gut dysbiosis. Probiotics are microorganisms similar to the beneficial bacteria found in the human gut, and they can help to restore the balance of the microbiome. Prebiotics are food for bacteria, they stimulate the growth and balance of beneficial bacteria (Barko PC, et al 2018).

*It is important to note that while fermented foods can be beneficial for the gut microbiome, they may also increase histamine levels in the body. Histamine is a chemical involved in the immune response, and it is produced by certain bacteria in the gut as well as by the cells in the body. High levels of histamine can be problematic for individuals who are sensitive to histamine or who have conditions such as histamine intolerance or mast cell activation syndrome. Therefore, it is important to speak to a healthcare professional before including fermented foods into your diet. Remember that at Nutrifix we can assess your nutrition according to your genetics and histamine is one of the first things we look at in our genetic and metabolic optimization approach.
As you may now know, your microbiome is very important for your health, as it influences your digestion, metabolism and overall health. Remember to have a nutritious, balanced diet, to keep active, to implement tools for light exposure and to manage stress. Contact us to help you select optimal habits according to your genes and take your health to the next level.